

Allergic asthma is a common inflammatory condition that affects the small tubes carrying air in and out of the lungs, known as the airways or bronchi. Airways of asthmatic individuals are generally more sensitive than normal and overreact to various stimuli. When an allergic individual with asthma comes into contact with a trigger (something that irritates the airway, i.e. pollen, dust), the lining of the airways becomes inflamed and the muscles around the walls tighten so that the airways become narrower and glands in the airways produce large amounts of mucus.
The prevalence of asthma is increasing. In 2009, 300 million people were affected worldwide. Approximately 5.4 million people in the UK are currently being treated for asthma. Approximately one in 11 children and one in 12 adults now have asthma.
London Allergy Care & Knowledge provides testing and treatment plans for children and adults who experience allergic asthma. We provide specialised and personalised treatments such as Sublingual Immunotherapy to aeroallergens (pollens, house dust mite, animals and moulds) in order to desensitise from allergens that cause allergic asthma.

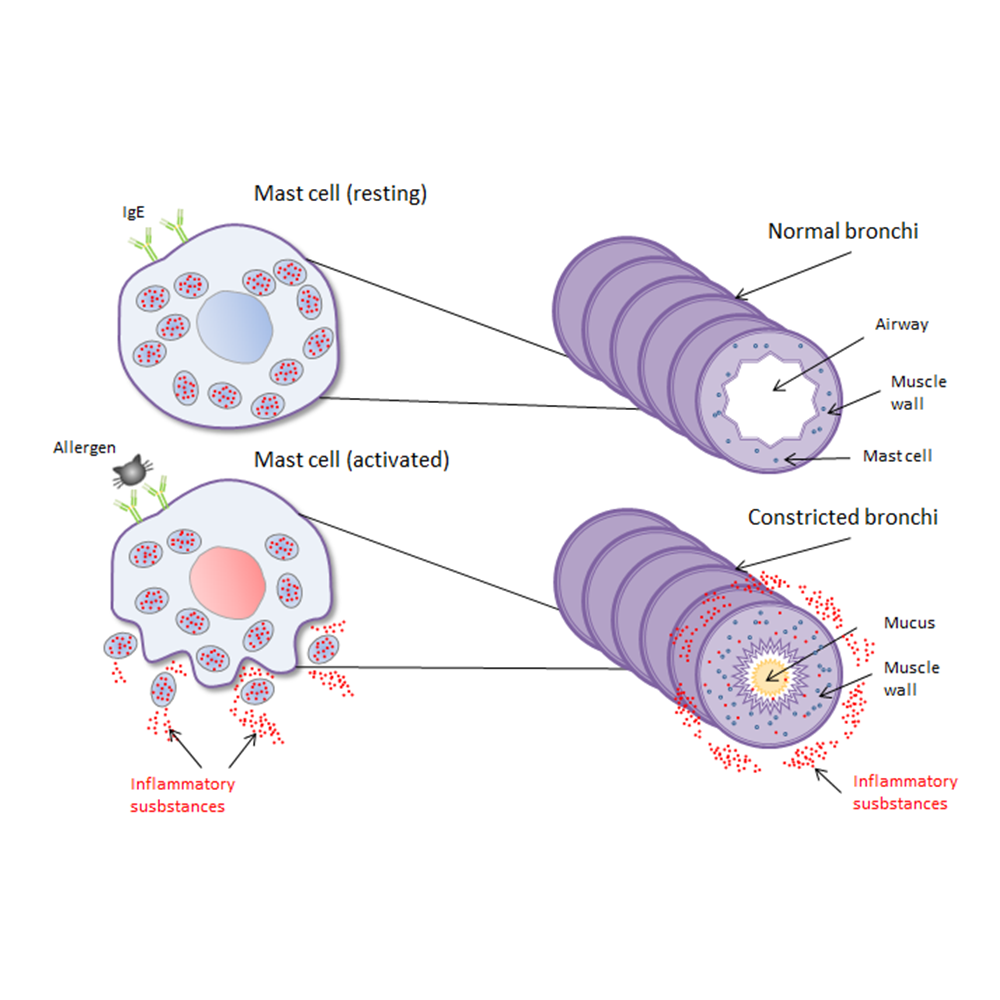
There are numerous mast cells in the airways of the lungs (blue dots). When they meet an allergen, they mistakenly consider it a harmful substance. In response, they release histamine and other chemicals that cause constriction and swelling of the airway. This results in acute asthma symptoms. Chronic exposure to allergens, such as cat dander or house dust mite, can lead to chronic inflammation , and therefore,chronic symptoms of asthma.
The most common allergens that cause attacks are:
- Pollen (grass and tree)
- Dust mites
- Pet dander
The chronic inflammation caused by allergen exposure is characterised by a type of airway inflammation called T-Helper 2 inflammation.
There are different patterns of asthma. Some individuals have self-limited episodes followed by extended symptom-free periods. This is called intermittent asthma. Meanwhile, patients with seasonal allergic asthma have symptoms for longer periods of time and they are related to the exposure to seasonal outdoor inhalant allergens (i.e. grasses or trees). Lastly, patients with chronic or persistent asthma have daily or very frequently recurring symptoms. Usually, their symptoms result in impairment of daily activities.
Asthma has a variable course. Many children with asthma see it improve as they get older. However, in some individuals, asthma persists into adult life. Whatever the course, asthma is virtually always controllable . The disease is characterised by variable and recurring symptoms due to airflow obstruction. The severity of the disease is variable and can range from trivial and infrequent in some – to severe, unremitting and dangerous in others.


Patients with asthma may have one or more of the following symptoms:
- Repeated short cough that occurs most frequently during the night and early morning hours .
- Recurring wheezing. Wheezing is a whistling sound that occurs when the airways are obstructed.
- Rapid breathing. During airway obstruction, asthmatic subjects may breathe faster than normal.
- Feeling breathless. Patients with asthma may gasp for breath.
- Chest tightness. Asthmatic subjects may experience a sensation rather like having a band tightening around the chest.
- Laboured breathing. In some patients, especially younger infants and children, difficulty with breathing may be observed with rapid abnormal movements of the chest. During airway obstruction, the ribs and clavicle may be more visible as the patient makes greater effort to inhale and exhale.
Asthma symptoms vary widely in young children. Coughing is often the only symptom.
The cause of asthma is not well understood, but is it clear that asthma often runs in families.
Family history is one of the major risk factors for the condition. Parents with asthma are more likely to have children with asthma. If asthma is present in both parents, the likelihood of a child having asthma is even greater, but even then not all of the children will have asthma. There are a number of genes which have been identified in association with asthma.This suggests that there is some additional factor that we do not yet fully understand, other than inheritance that influences the development of asthma.
A trigger is anything in the environment that causes the irritation, inflammation and narrowing of the airways. There are two categories of triggers: allergic (pollens, house dust mites, animal dander) and non-allergic (temperature, exercise, smoke, viral infections, combustion products, etc.).
Some risk factors for the development of asthma have been identified, such as the presence of other related allergic conditions (known as atopic conditions, i.e. eczema, hay fever, food allergy, etc); having bronchiolitis as a child; exposure to tobacco smoke as a child, particularly if your mother smoked during pregnancy; being born prematurely or with a low birth weight.
It has also been suggested that differences in macronutrient and micronutrient dietary content, as well as alterations in the gut microbiome, could explain the increase in allergies.


Some risk factors for the development of asthma have been identified, such as the presence of other related allergic conditions (known as atopic conditions, i.e. eczema, hay fever, food allergy, etc); having bronchiolitis as a child; exposure to tobacco smoke as a child, particularly if your mother smoked during pregnancy; being born prematurely or with a low birth weight.
Also, it has been suggested that differences in macronutrient and micronutrient dietary content and alterations in the gut microbiome could explain the increase in allergies.
